Note: If you're short on time and just want to try it, follow this link on any device and click "Chart a Local Anesthesia Case": case.xchart.com
Many providers, especially dentists, do local anesthesia at their practices all day, every day. If a dentist gives local anesthetic to eight patients per work day for 180 work days in a year, that's over 1,400 patients anesthetized per year! And that's not even including patients that require local anesthetic for periodontal procedures performed by hygienists.
In short, dentists/hygienists do a lot of local anesthesia.
You don't have to be a statistician to know that the more you do something, the more likely you are to encounter a complication. While we might disagree on what should be considered a "serious complication" we can all agree that a patient going to the hospital secondary to having local anesthesia administered—is a serious complication. That would likely be one of the worst days of your career, especially if we are talking about a pediatric patient.
No one wants their patient to experience any complications but it does happen. We have been disheartened by many reports of patients being harmed by inappropriate dosing of local anesthetic, the worst of which lead to death. Thankfully, those are quite rare, but many dental lawsuits and dental board disciplinary cases involve inappropriate administration of local anesthetic often coupled with inadequate documentation of local anesthetic among other things.
How would you feel if your documentation of local anesthetic was being reviewed by the dental board right now? Would you feel confident or would you be sweating a bit?
I think it's safe to say, for many of us, we could probably do better than we do currently. What if it were simple to do better? But let's be clear, it's anything but simple.
I'm sure you pride yourself in the quality of the procedures you perform, but how good are your mental math skills? To do this right, you have to (be proficient at) converting a percentage to (milligrams per milliliter), multiplying that by milliliters in decimal form, cataloguing that number mentally as well as noting the time, mentally determining what percentage that number is in relation to the mass of the patient and do that all over again for every injection and every type of local anesthetic and keep a running tally! What about really long cases where local anesthetic starts to wear off? Now elimination half-life comes into play and then you have to recall the reported elimination half-lives of each local anesthetic in relation to when you have each dose. That takes some log2 based calculus to evaluate! To make matters even more worse, everything varies. Guidelines vary by age group and patient mass, and elimination half-life of drugs varies drastically. But to really know, and this is very important, you have to take into account the combined toxicity of all the LA you have given.
Let's review the challenge:
- Local anesthetic drugs vary in elimination half-life
- Guidelines vary by age group
- You need a different elimination half-life calculations for each dose given of each drug
- Guidelines are stated in milligrams, but many providers count cartridges
- If using multiple types of drugs, you have to sum up their total combined toxicity
- If things go wrong, emergency rooms need to know how many milligrams of each drug were given and when
- Cartridges are 1.8mL, concentration is stated as a percentage, milligrams of drug per cartridge varies by concentration and there are multiple different concentrations available.
- Some providers even dilute local anesthetics which further complicate the formulas
Can you confidently tell me that you know exactly how many more "carps" of a given local anesthetic you can give 1.5 hours into your case and still be within guidelines?
If we're honest with ourselves: this is impossible to do in your head.
So, we compensate
Most of us learn to simplify all of this into a mental model where we can be relatively sure we're not going over any toxic limits. But really, are you 100% sure? We've found that many dental providers can't even confidently report how many milligrams of actual drug was administered, let alone know how that stacks up to recommendations at a given point in the case. "Carpules" are not a valid dosing unit. Even so, they won't mean anything to the ER doctor if, God forbid, your patient ends up there.
To make matters worse, when your patient is already sedated if that's what you're doing, the early warning signs of adverse reactions to too much local anesthetic can be even harder to spot!
Enter computers. Not only can computers do all that math for you they can compute the exact dose you can give and re-compute it every second continuously without even breaking a sweat!
Computers can help you do the math like a superhero! So you can confidently focus on your procedure.
We at AnesthesiaCharting.com have a tool that we want to share with you and every provider for that matter. We felt we could make a positive difference and we felt so passionate about it that we decided to offer our local anesthetic tracking software ABSOLUTELY FREE to anyone. Period. No catch. No ads.
How can I use it?
Our AnesthesiaCharting.com local anesthetic tracker can be used on a PC, Mac, tablet, phone, iOS, Android or anything that runs a modern browser like Chrome, Edge, or Safari with out ever having to download an app. You don't even need to create an account!
Follow this link and click "Chart a Local Anesthesia Case" to try it for yourself: case.xchart.com
You start by entering a patient's DOB, weight and height. It automatically calculates the BMI and assesses the age of the patient to select whether manufacturer's guidelines or American Academy of Pediatric Dentistry are utilized. You can then choose the types of LA that you plan to use. As you administer each local anesthetic, simply type in the administered amount of LA either as cartridge, mg, or mL form (whichever you are using).
Our software then tracks:
- Administration time
- Total amount administered
- Total of each local anesthetic as well as total epinepherine reported in milligrams.
It then uses this info to calculate in real time:
- An estimated systemic local anesthetic toxicity percentage for all doses combined.
- This percentage is recalculated every second in accordance with the half-life elimination rate of each local anesthetic separately and then jointly.
- How much more of each drug you can give without exceeding guidelines in your preferred unit based on this particular patient's age/weight.
Each selected anesthetic will have an entry that looks like this:
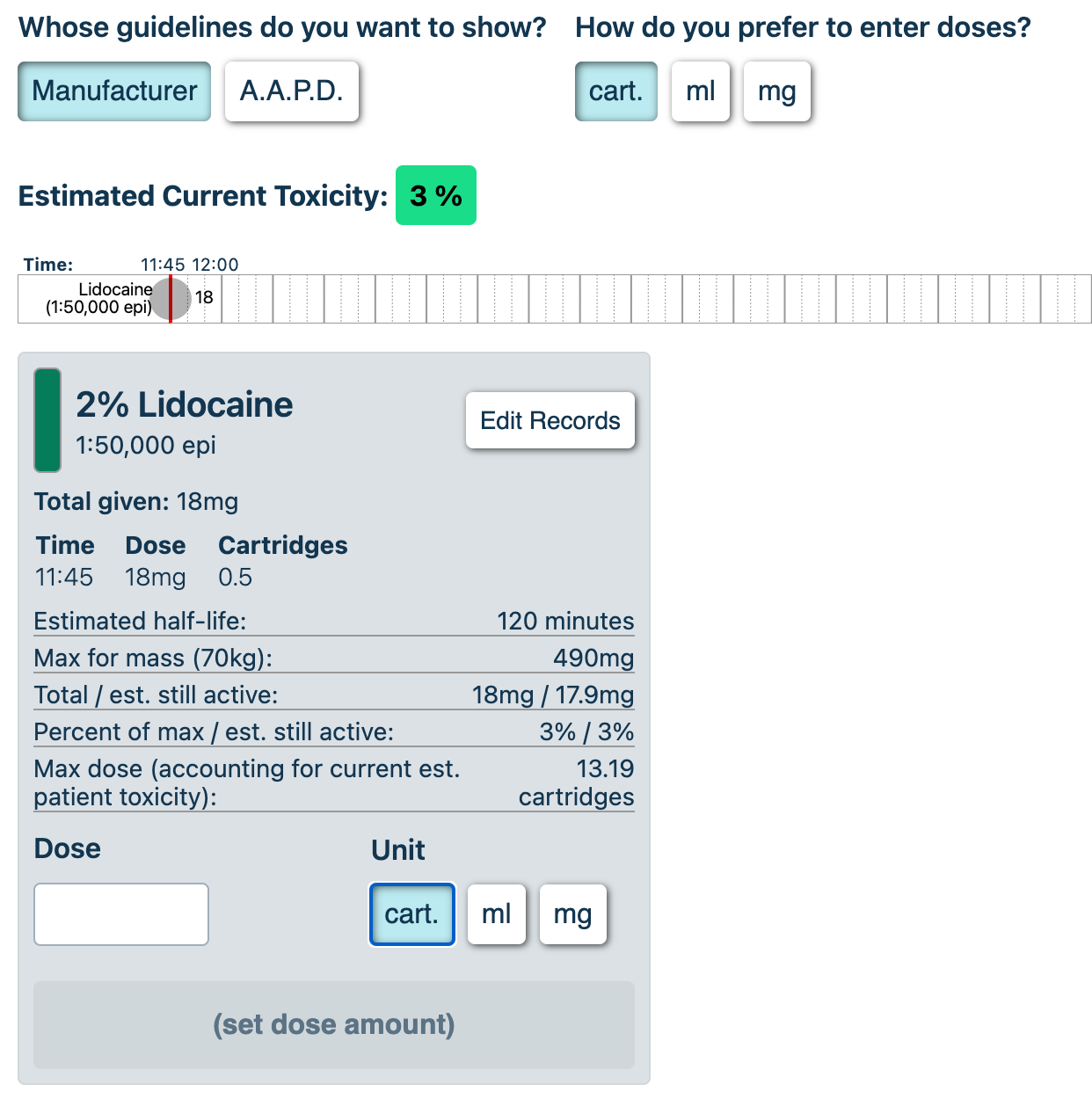
Ultimately, this is a tool to help providers know when they are nearing or have exceeded guideline amounts of local anesthetic per the statistical norms associated with the weight and age of the patient.
Getting this data into your charting system
But not only that! It's super easy to drop this into any digital charting system. See this quick clip for a demo of that:
We've heard from providers, especially those who do really long cases, that they love knowing how much local anesthetic can safely be re-administered near the end of a procedure. Speaking of lengthy cases, very few providers record the time of administration of local anesthetic whereas most providers tally the total amount of local anesthetic administered during a case and record those totals at the end of the case but, is that accurate? Think through the worst case scenario where a patient underwent a lengthy appointment at your office and local anesthetic was administered several times throughout the procedure. An unforeseen complication resulted from treatment that led to litigation. Your records indicate the total tally of local anesthetic administered as it was tabulated at the end of the case. Now, you know that you didn't give that entire tabulation of LA as a one time bolus, but if your records don't indicate otherwise, how will you defend that?
AnesthesiaCharting.com is here to help you make tracking and reporting administered local anesthetic simple. We are here to make you do math like a superhero. Most of all, our ultimate goal is to make things safer for your patients and easier for you the provider.
This is just another example of how we're on your side trying to make it simple to do the right thing.
Again, here's the link, click "Chart a Local Anesthesia Case" to use it for yourself: case.xchart.com.